Diabetic Retinopathy
Diabetic Retinopathy Specialists in Wilmington
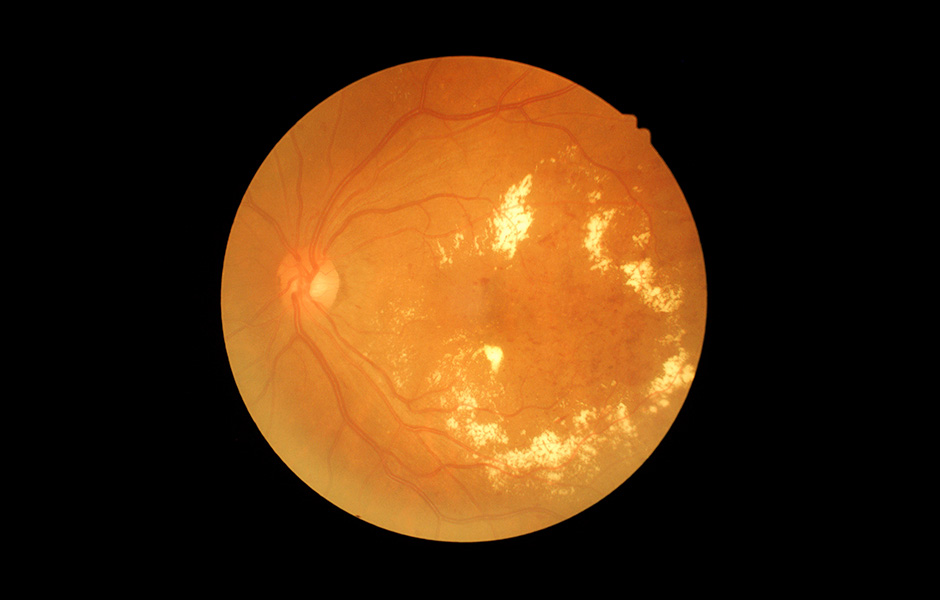
What Is Diabetic Retinopathy?
Diabetes damages the body’s normal circulation, which is why people with diabetes may have problems with circulation to their legs, kidneys, heart, brain and eyes. At least 50 percent of all diabetics will develop diabetic retinopathy (abnormal retinal blood circulation), and the incidence increases with the duration of the disease. After 20 years, more than 90 percent of diabetics have some degree of diabetic change.
Diabetic retinopathy is a leading cause of blindness in the United States in middle-aged adults. Fortunately, new methods of treatment in recent years have decreased blindness among diabetics and have increased the possibility of retaining useful vision.
Types of Diabetic Retinopathy
There are two main types of diabetic retinopathy: nonproliferative and proliferative:
Nonproliferative Diabetic Retinopathy
In nonproliferative diabetic retinopathy, there is leakage caused by damage to small retinal blood vessels (capillaries). This leakage allows proteins and lipids from the blood to accumulate in the retina, causing swelling. If this swelling occurs in the area of central vision (macular edema), sight may be significantly diminished. As the disease progresses, retinal capillaries may also become closed off, resulting in poor retinal nutrition. Lack of circulation to the center of vision (macular ischemia) can result in severe and permanent loss of central vision.
Proliferative Diabetic Retinopathy
When there is widespread impairment of retinal nutrition due to capillary leakage and closure, proliferative diabetic retinopathy develops. The poorly nourished retina sends out a chemical “distress signal” which causes new blood vessels to grow (proliferate) on the retinal surface. Unfortunately, these new blood vessels are very fragile and often rupture, allowing bleeding to occur within the eye (vitreous hemorrhage). Scar tissue can also grow around the abnormal blood vessels, which may lead to retinal detachment and possible permanent blindness. The proliferative form of diabetic retinopathy is present in approximately 20 percent of patients with diabetes of 10-year duration.
Widespread impairment of retinal blood circulation leads to the development of new, fragile blood vessels. Large clinical trials have shown that a procedure called scatter laser photocoagulation can be effective in halting or reversing new vessel growth. Many eyes, even without visual problems, need to begin laser treatments if there are certain abnormal vessels present. Those eyes, having no visual problems, must be detected by examination. Overall, the incidence of blindness over two years can be reduced by 66 percent for eyes with new vessels on the optic nerve and by 37 percent for eyes with new vessels in other locations. The laser treatment consists of applying multiple laser burns, often divided into several sessions, to the peripheral retina. Although mildly uncomfortable, the treatment usually can be done without the need for local anesthesia. The main complications from treatment are loss of some peripheral vision, a decrease in night vision, occasionally some loss of central vision, and possible mild enlargement of the pupil. If laser treatment is needed, the risk factors of not being treated are much higher than the risk of being treated.
Again, a new class of medications targeting vascular endothelial growth factor (VEGF) produced by poorly nourished retina can be directly injected into the eye. The anti-VEGF drugs Avastin™ and Lucentis™ have been used with good results in managing proliferative diabetic retinopathy, often along with scatter laser photocoagulation treatment.
Symptoms

In the early stages of diabetic retinopathy, there are usually no symptoms. Therefore, it is very important that all patients with diabetes have a comprehensive dilated eye examination at least once a year before any symptoms develop. During this exam, your retinal specialist can check for any signs of damage to the retina and optic nerve, including leaking blood vessels, swelling of the macula and growth of new vessels. To help prevent the development and progression of diabetic retinopathy, patients are urged to control their blood sugar, blood pressure and cholesterol levels.
Treatment
Good control of diabetes with intensive management and control of blood sugar will delay, and possibly prevent, both the development and progression of diabetic retinopathy. Patients with diabetic retinopathy frequently need to have special photographs of the retina taken. This series of photos is called fluorescein angiography (FA).
Laser photocoagulation directed at the retina to seal living blood vessels in patients with background diabetic retinopathy. Panretinal photocoagulation consists of laser spots scattered through the sides of the retina to reduce abnormal blood vessel growth (neovascularization) and help seal the retina to the back of the eye in patients with proliferative diabetic retinopathy. This can help prevent retinal detachment. There is little recuperation needed after laser surgery for diabetic retinopathy. Laser surgery may require more than one treatment to be effective.
Vitrectomy surgery is scheduled for patients with very advanced proliferative diabetic retinopathy or retinal detachment. In vitrectomy surgery, your physician removes the blood-filled vitreous and replaces it with a clear solution. This allows light to pass through the clear fluid to the retina, where the images are conveyed to the brain.
Pharmacotherapy: Increasingly, a variety of medications are being used to treat the manifestations of background and proliferative diabetic retinopathy. These involve intravitreal injections of small amounts of medication into the eye.
The type of retinopathy, as well as the patient’s general health and eye structure, will determine the kind of treatment needed and the type of anesthesia utilized.

